Module 1: Foundations of Infection Control, Safety, and Compliance

The content is designed for licensed and non-physician professionals working in regulated environments, including aesthetic practitioners, technicians, and clinical support personnel.
By the end of this module, participants will understand how infection spreads, how to interrupt transmission pathways, and how to implement safe, compliant practices in daily professional activities.
This module introduces the fundamental principles of infection control, safety, and regulatory compliance in healthcare-adjacent and outpatient practice environments. It is designed to provide foundational knowledge necessary to minimize risk, prevent cross-contamination, and ensure safe professional practice.
Infection control is a critical component of all patient-facing and procedure-based services. In the United States, failure to follow proper infection prevention protocols can result in serious health risks, including transmission of bloodborne pathogens such as Hepatitis B (HBV), Hepatitis C (HCV), and Human Immunodeficiency Virus (HIV).
According to the Centers for Disease Control and Prevention (CDC), improper infection control practices have been directly linked to multiple outbreaks in outpatient settings. These incidents highlight the necessity of structured education and strict adherence to standardized protocols. This module focuses on practical, real-world application of infection control measures, including hand hygiene, personal protective equipment (PPE), instrument handling, environmental sanitation, and regulatory awareness.
Learning Objectives

Upon completion of this module, participants will be able to:
1. Explain the fundamental principles of infection transmission, including contact, droplet, and airborne pathways.
2. Identify common sources of contamination in outpatient and healthcare-adjacent environments, including surfaces, instruments, and human contact.
3. Demonstrate proper hand hygiene techniques based on CDC guidelines, including when and how to perform handwashing and hand antisepsis.
4. Select and correctly use personal protective equipment (PPE), including gloves, masks, and protective barriers, based on risk level and type of procedure.
5. Describe proper cleaning, disinfection, and sterilization processes, and differentiate between these levels of decontamination.
6. Recognize the risks associated with bloodborne pathogens, including HIV, HBV, and HCV, and understand basic prevention strategies.
7. Apply standard precautions in daily practice to reduce the risk of cross-contamination and infection transmission.
8. Understand the importance of regulatory compliance and the role of infection control protocols in maintaining safe practice environments.
9. Identify unsafe practices and correct them using evidence-based infection control principles.
10. Integrate infection prevention strategies into routine workflow in order to protect both clients and practitioners.
Core Concepts: Principles of Infection Transmission
Infection transmission occurs when microorganisms are transferred from a source to a susceptible host. Understanding how infections spread is essential for preventing contamination in professional environments.
There are three primary modes of transmission:
1. Contact Transmission
This is the most common form of infection spread. It occurs through direct contact (person-to-person) or indirect contact (via contaminated surfaces or instruments). For example, using non-sterile tools or touching a client without proper hand hygiene can lead to transmission.
2. Droplet Transmission
This occurs when respiratory droplets containing microorganisms are expelled through coughing, sneezing, or speaking. These droplets can travel short distances and land on mucous membranes (eyes, nose, mouth) of another person.
3. Airborne Transmission
This involves smaller particles that remain suspended in the air for longer periods and can be inhaled. While less common in aesthetic environments, it is still relevant in enclosed or poorly ventilated spaces.


Chain of Infection
Infection transmission follows a predictable sequence known as the chain of infection. It includes:
• Infectious agent (bacteria, virus, fungi)
• Reservoir (where the organism lives)
• Portal of exit
• Mode of transmission
• Portal of entry
• Susceptible host
Breaking any link in this chain prevents infection.
For example, proper hand hygiene removes microorganisms (agent), while gloves create a barrier (mode of transmission), and surface disinfection eliminates reservoirs.
According to CDC guidelines, consistent use of standard precautions can significantly reduce infection risk in outpatient environments.
Hand Hygiene and Infection Prevention
Hand hygiene is the single most effective measure to prevent the spread of infections in any healthcare or procedure-based environment. Contaminated hands are one of the primary sources of cross-contamination between clients, surfaces, and instruments.
According to the Centers for Disease Control and Prevention (CDC), proper hand hygiene can reduce the transmission of infectious agents by up to 50%.

There are two primary methods of hand hygiene:
1. Handwashing with soap and water
This method physically removes dirt, organic material, and microorganisms from the skin.
Handwashing must be performed:
• Before and after each client interaction
• After contact with blood or bodily fluids
• After removing gloves
• After touching contaminated surfaces
The recommended duration is at least 20 seconds, ensuring coverage of all areas including palms, back of hands, between fingers, and under nails.
2. Alcohol-based hand sanitizer
This method rapidly reduces the number of microorganisms on the skin.
It should be used:
• When hands are not visibly soiled
• Before and after procedures
• Between client contacts when handwashing is not immediately available
However, it is not effective against all pathogens and should not replace handwashing when contamination is visible.

Common Mistakes
Failure to perform hand hygiene at the correct time
Insufficient duration (less than 20 seconds)
Missing areas such as thumbs and fingertips
Improper glove use as a substitute for hand hygiene
It is critical to understand that gloves do not replace hand hygiene. Hands must be cleaned before putting on gloves and after removing them.
Consistent adherence to proper hand hygiene protocols significantly reduces the risk of infection transmission and is a fundamental requirement for safe and compliant practice.
Personal Protective Equipment (PPE)
Personal Protective Equipment (PPE) is a critical component of infection prevention and control. It serves as a barrier between the practitioner and potential sources of contamination, reducing the risk of exposure to infectious agents.
The selection of PPE depends on the level of risk associated with the procedure, the type of exposure anticipated, and the environment in which services are performed.

Common Types of PPE
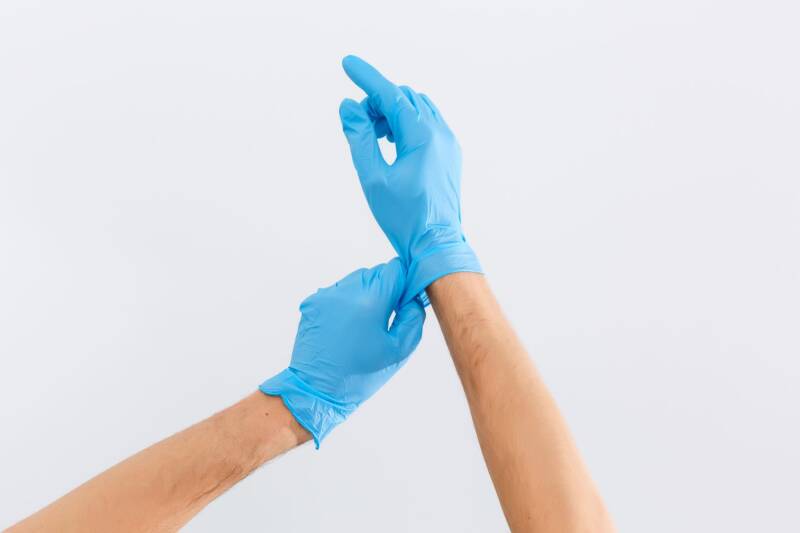
Gloves
Gloves are used to prevent direct contact with blood, bodily fluids, mucous membranes, and contaminated surfaces.
Key principles:
• Must be worn during all procedures involving potential exposure
• Must be changed between each client
• Must never be reused
• Hands must be cleaned before and after glove use

Masks
Masks protect the nose and mouth from droplets and reduce the risk of inhaling infectious particles.
They should be used:
• During close-contact procedures
• When there is a risk of splashes or sprays
• In environments with limited ventilation
Eye Protection (Goggles or Face Shields)
Protects the eyes from exposure to droplets or splashes.
Recommended when:
• Performing procedures with potential fluid exposure
• Working in close proximity to the client’s face


Protective Clothing
Includes gowns or protective garments designed to prevent contamination of clothing and skin.
Use is recommended:
• During procedures with a higher risk of contamination
• When contact with bodily fluids is possible
Proper Use of PPE
PPE must be used correctly to be effective. Improper use can increase, rather than decrease, the risk of contamination.
Important guidelines:
• Always put on PPE before starting a procedure
• Remove PPE carefully to avoid self-contamination
• Dispose of single-use PPE immediately after use
• Never touch face or personal items while wearing contaminated PPE

PPE is not a substitute for proper infection control practices.
It must be used in combination with:
• Hand hygiene
• Surface disinfection
• Proper instrument handling
Failure to follow these combined measures can result in infection transmission even when PPE is used.
The consistent and correct use of PPE significantly reduces occupational risk and is a key requirement in regulated professional environments.
Cleaning, Disinfection, and Sterilization
Effective infection control requires a clear understanding of the three levels of decontamination: cleaning, disinfection, and sterilization. Each level serves a different purpose and must be applied correctly based on the type of equipment and risk of exposure.


Disinfection
Disinfection eliminates many or all pathogenic microorganisms, except bacterial spores, on inanimate objects.
There are different levels of disinfection:
• Low-level disinfection
Used for non-critical surfaces (e.g., countertops, chairs)
• Intermediate-level disinfection
Effective against most viruses and bacteria, including some resistant organisms
• High-level disinfection
Used for instruments that come into contact with mucous membranes
Disinfection must follow manufacturer guidelines regarding:
• Contact time
• Concentration
• Application method
Failure to follow these instructions reduces effectiveness.
Cleaning
Cleaning is the physical removal of visible debris, organic material, and microorganisms from surfaces and instruments. It is the first and most essential step before any disinfection or sterilization process.
Key points:
• Removes dirt, blood, and organic matter
• Reduces microbial load
• Must always be performed before disinfection or sterilization
Without proper cleaning, disinfectants and sterilizing agents may not be effective.


Sterilization
Sterilization is the highest level of decontamination. It destroys all microorganisms, including bacteria, viruses, fungi, and spores.
Methods include:
• Steam sterilization (autoclave)
• Chemical sterilization
• Dry heat (less common)
Sterilization is required for critical instruments that penetrate skin or come into contact with sterile body areas.
Critical Concepts
Not all tools require sterilization. The level of processing depends on classification:
• Non-critical items → cleaning + low-level disinfection
• Semi-critical items → high-level disinfection
• Critical items → sterilization

Common Errors
- Skipping the cleaning step
- Incorrect contact time for disinfectants
- Reusing single-use items
- Improper storage of sterilized instruments
These errors significantly increase infection risk.
Proper implementation of cleaning, disinfection, and sterilization protocols is essential for maintaining safe practice environments and ensuring regulatory compliance.
Practical Application in Professional Settings
The principles of infection control must be consistently applied in real-world practice environments. Understanding theory is not sufficient without the ability to implement these measures in daily workflow. In outpatient and healthcare-adjacent settings, practitioners are responsible for maintaining a clean, controlled, and safe environment for every client interaction.


Key practical applications
- Preparing the workspace before each client, including surface disinfection and organization of sterile or clean instruments
- Performing hand hygiene before and after every client interaction, regardless of perceived contamination
- Using appropriate PPE based on the procedure and level of exposure risk
- Avoiding cross-contamination by maintaining separation between clean and contaminated items
- Proper disposal of waste materials, including single-use items and potentially contaminated supplies
- Ensuring all reusable instruments undergo appropriate cleaning, disinfection, or sterilization
- Maintaining awareness of high-touch surfaces and disinfecting them regularly
Module Summary
This module introduced the foundational principles of infection control and prevention in regulated practice environments.
Participants learned:
- How infections are transmitted and how to interrupt the chain of infection
- The critical role of hand hygiene in preventing cross-contamination
- The proper selection and use of personal protective equipment (PPE)
- The differences between cleaning, disinfection, and sterilization
- How to apply infection control protocols in real-world professional settings
The consistent application of these principles is essential for protecting both clients and practitioners, maintaining safe environments, and ensuring compliance with established safety standards.
Infection prevention is a core responsibility of every professional working in a procedure-based setting and serves as the foundation for all further training modules.

