Module 7: Oral Health and Systemic Safety

Oral health is a critical component of overall health and safety. The condition of the oral cavity is closely linked to systemic health, infection risk, and the prevention of disease transmission.
Poor oral hygiene is not limited to cosmetic concerns. It can lead to serious conditions such as periodontal disease, bacterial infections, and systemic complications affecting the cardiovascular and immune systems.
In healthcare-adjacent and outpatient environments, professionals must understand how oral health influences overall safety, particularly in procedures involving close facial contact, mucous membranes, and potential exposure to biological fluids.
This module provides foundational and practical knowledge on oral hygiene, disease prevention, and the relationship between oral health and systemic safety.
Learning Objectives
Upon completion of this module, participants will be able to:
- Explain the relationship between oral health and systemic health
- Identify common oral diseases, including dental caries and periodontal disease
- Describe proper daily oral hygiene practices
- Understand recommended dental care schedules for different age groups
- Recognize signs of oral infection and when to refer clients
- Understand how poor oral hygiene increases infection risk
- Apply oral health awareness in professional safety practices
- Educate clients on basic oral hygiene and preventive care
- Identify risk factors affecting oral and systemic health
- Integrate oral health awareness into safety and prevention strategies
Core Concepts: Oral Health and Systemic Connection
The oral cavity contains a complex microbiological environment. When oral hygiene is poor, bacteria can accumulate and lead to infection and inflammation.
These bacteria may enter the bloodstream and contribute to systemic conditions such as:
• Cardiovascular disease
• Diabetes complications
• Respiratory infections
• Chronic inflammation
Periodontal disease, in particular, has been linked to increased systemic inflammatory response, which can negatively impact overall health.
Maintaining oral hygiene is therefore not only a dental concern, but a public health and systemic safety issue.


Daily Oral Hygiene Practices
Tooth Brushing
Tooth brushing is the foundation of oral hygiene and must be performed correctly to be effective.
• Brush 2 times per day (morning and before sleep)
Brushing in the morning removes bacteria accumulated overnight, while brushing before sleep is critical to eliminate plaque and food debris before prolonged inactivity.
• Use fluoride toothpaste
Fluoride strengthens enamel, enhances remineralization, and helps prevent the development of cavities.
• Duration: at least 2 minutes
Adequate time ensures that all areas of the mouth are properly cleaned. Rushing often leads to missed zones, especially posterior teeth.
• Use gentle circular motions at a 45° angle to the gumline
This technique (Bass method) allows the bristles to reach slightly below the gumline, effectively removing plaque from areas where periodontal disease commonly begins.
• Clean all surfaces: outer, inner, and chewing surfaces
Special attention should be given to:
– inner surfaces of front teeth (use vertical strokes)
– molars and hard-to-reach posterior areas
– gumline, where plaque tends to accumulate
Additional considerations:
• Avoid excessive pressure, which can cause enamel wear and gum recession
• Replace toothbrush every 3–4 months or sooner if bristles are worn
• Consider using an electric toothbrush for improved plaque removal and consistency


Flossing
Flossing is a critical component of oral hygiene that complements tooth brushing by cleaning areas that toothbrush bristles cannot reach, particularly between teeth and below the gumline.
• Perform once daily
Daily flossing is sufficient to disrupt plaque formation in interproximal areas. It is most effective when performed before brushing at night, allowing fluoride toothpaste to better access cleaned surfaces.
• Removes plaque and debris between teeth
Dental floss mechanically removes food particles and bacterial biofilm from tight spaces between teeth and along the gumline. These areas are highly susceptible to plaque accumulation due to limited access during brushing.
• Essential for preventing gum disease
Failure to remove plaque interproximally can lead to gingival inflammation (gingivitis), which may progress to periodontitis if untreated. Regular flossing helps reduce bleeding, inflammation, and pocket formation, supporting overall periodontal health.
Additional considerations:
• Use proper technique: gently guide floss between teeth using a sawing motion, then curve it into a “C” shape around each tooth
• Avoid snapping floss into the gums to prevent tissue injury
• Consider alternatives such as floss picks, interdental brushes, or water flossers for patients with braces, implants, or limited dexterity
Mouthwash
Mouthwash is a supportive component of oral hygiene that enhances, but does not replace, mechanical plaque removal through brushing and flossing. It provides additional chemical control of bacteria and can target specific oral health concerns.
• Use as an adjunct (not a replacement)
Mouthwash should be used in combination with brushing and flossing, not as a substitute. Mechanical removal of plaque remains the primary method of maintaining oral hygiene, while mouthwash serves as an additional preventive measure.
• Helps reduce bacterial load
Antimicrobial mouthwashes can reduce the number of bacteria in the oral cavity, particularly in hard-to-reach areas. This can help decrease the risk of plaque accumulation, gingival inflammation, and halitosis (bad breath).
• Can support gum health
Certain formulations (e.g., chlorhexidine, essential oils) have been shown to reduce gingivitis and improve overall periodontal health when used as directed. Therapeutic mouthwashes may be recommended in cases of inflammation or after dental procedures.
Additional considerations:
• Choose the appropriate type:
– Fluoride rinses for cavity prevention
– Antimicrobial rinses for gum health
– Alcohol-free options for patients with dry mouth or sensitivity
• Avoid eating or drinking for at least 30 minutes after use to allow active ingredients to remain effective
• Do not overuse medicated mouthwashes (especially chlorhexidine), as prolonged use may cause staining or alter taste perception


Common Mistakes
Even when individuals maintain a regular oral hygiene routine, improper technique or inconsistency can significantly reduce its effectiveness and increase the risk of oral disease.
• Brushing too quickly
Rushing through brushing often results in incomplete plaque removal, especially in hard-to-reach areas such as posterior teeth and along the gumline. Brushing for less than the recommended 2 minutes commonly leads to missed surfaces and uneven cleaning.
• Applying excessive pressure
Using too much force does not improve cleaning efficiency and can cause harm. Overbrushing may lead to enamel wear, increased tooth sensitivity, and gingival recession, exposing root surfaces and increasing vulnerability to decay.
• Skipping flossing
Neglecting interdental cleaning allows plaque and food debris to accumulate between teeth, where toothbrush bristles cannot reach. This significantly increases the risk of gingivitis, periodontal disease, and interproximal caries.
• Inconsistent routine
Irregular oral hygiene habits reduce long-term effectiveness. Skipping brushing sessions or performing hygiene inconsistently allows bacterial biofilm to mature and become more difficult to remove, leading to increased risk of inflammation and disease progression.
Dental Care Recommendations by Age
Children
• First dental visit: by age 1
• Regular visits: every 6 months
• Supervised brushing recommended
Adults
• Dental check-ups: every 6 months
• Professional cleaning: every 6 months (or as needed)
• Increased frequency if risk factors present
High-Risk Individuals
More frequent monitoring required for:
• Smokers
• Diabetic patients
• Individuals with gum disease history
• Immunocompromised individuals

Common Oral Diseases

Dental Caries (Cavities)
Dental caries is a chronic, multifactorial disease characterized by the progressive destruction of tooth structure due to bacterial activity. It is one of the most common oral health conditions and is largely preventable with proper hygiene and dietary control.
• Caused by bacterial breakdown of enamel due to plaque accumulation
Oral bacteria metabolize fermentable carbohydrates (especially sugars) and produce acids as a byproduct. These acids lower the pH in the oral environment, leading to demineralization of enamel. When plaque is not effectively removed, this process continues, resulting in the formation of cavities.
Disease progression:
• Initial stage: Demineralization appears as white spot lesions on enamel
• Intermediate stage: Enamel breakdown leads to visible cavities
• Advanced stage: Decay progresses into dentin and may reach the pulp, causing pain and infection
Risk factors:
• Poor oral hygiene and plaque accumulation
• Frequent consumption of sugary or acidic foods and beverages
• Reduced saliva flow (dry mouth), which decreases natural protection
• Lack of fluoride exposure
• Irregular dental check-ups
Prevention:
• Regular brushing with fluoride toothpaste
• Daily flossing to remove plaque interproximally
• Limiting sugar intake and frequency of snacking
• Use of fluoride treatments or rinses when indicated
• Routine dental examinations and professional cleanings
Clinical significance:
If untreated, dental caries can lead to pain, infection, abscess formation, and eventual tooth loss. Early detection and intervention are essential to prevent complications and preserve tooth structure.
Gingivitis
Gingivitis is the earliest and most common stage of periodontal (gum) disease. It is a reversible inflammatory condition affecting the gingiva (gum tissue), primarily caused by the accumulation of bacterial plaque along the gumline.
• Early stage of gum disease characterized by inflammation and bleeding
Plaque buildup triggers an immune response in the gums, leading to redness, swelling, and bleeding, especially during brushing or flossing. At this stage, there is no irreversible damage to bone or connective tissue.
Common signs and symptoms:
• Red, swollen, or tender gums
• Bleeding during brushing or flossing
• Bad breath (halitosis)
• Shiny or puffy gum appearance
• Mild discomfort or sensitivity
Causes:
• Inadequate oral hygiene and plaque accumulation
• Improper brushing or flossing technique
• Hormonal changes (e.g., pregnancy)
• Smoking or tobacco use
• Certain medications or systemic conditions
Disease progression:
If untreated, gingivitis can progress to periodontitis, a more severe form of gum disease that involves destruction of supporting bone and connective tissue, potentially leading to tooth loss.
Prevention and management:
• Consistent brushing and flossing to remove plaque
• Regular professional dental cleanings
• Proper oral hygiene technique and education
• Use of antimicrobial mouthwash when indicated
• Addressing contributing risk factors (e.g., smoking cessation)
Clinical significance:
Gingivitis is fully reversible with proper care and early intervention. However, ignoring early symptoms increases the risk of progression to more serious periodontal disease.


Periodontitis
Periodontitis is an advanced stage of periodontal (gum) disease characterized by irreversible destruction of the supporting structures of the teeth, including connective tissue and alveolar bone. It develops as a progression from untreated gingivitis and can lead to tooth mobility and eventual tooth loss.
• Advanced gum disease that can lead to bone loss and tooth loss
Chronic inflammation caused by bacterial plaque triggers a destructive immune response, resulting in the breakdown of periodontal ligament and bone that support the teeth. As this support is lost, teeth may become loose and ultimately require extraction.
Key features:
• Formation of periodontal pockets (spaces between teeth and gums)
• Gum recession, exposing root surfaces
• Persistent inflammation and bleeding
• Tooth mobility or shifting
• Chronic bad breath (halitosis)
Disease progression:
• Early periodontitis: Mild attachment loss and pocket formation
• Moderate stage: Increased bone loss and deeper pockets
• Advanced stage: Significant bone destruction, tooth mobility, and possible tooth loss
Risk factors:
• Untreated gingivitis
• Poor oral hygiene and plaque accumulation
• Smoking (major contributing factor)
• Systemic conditions (e.g., diabetes)
• Genetic predisposition
• Stress and compromised immune response
Management and treatment:
• Professional deep cleaning (scaling and root planing)
• Improved daily oral hygiene (brushing, flossing, interdental cleaning)
• Antimicrobial therapy when indicated
• Surgical intervention in advanced cases
• Regular periodontal maintenance visits
Clinical significance:
Unlike gingivitis, periodontitis is not fully reversible. Early diagnosis and intervention are critical to slow disease progression, preserve remaining bone, and maintain tooth function.
Oral Infections
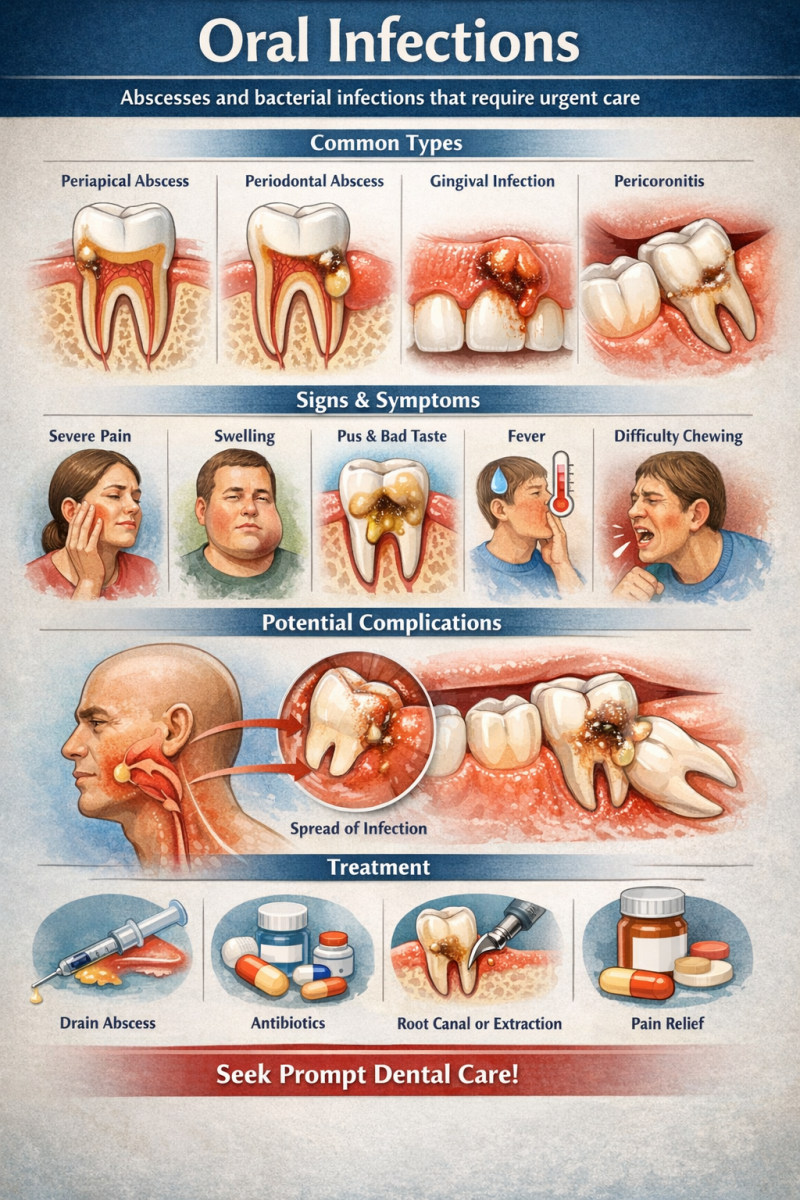
Oral infections are acute or chronic conditions caused by bacterial invasion of oral tissues. They may involve the teeth, gums, or surrounding structures and can rapidly progress if not treated promptly. Many oral infections require urgent professional care to prevent serious complications.
• May include abscesses and bacterial infections that require urgent care
A dental abscess is a localized collection of pus resulting from bacterial infection, often originating from untreated dental caries or advanced periodontal disease. These infections can spread beyond the oral cavity if not properly managed.
Common types:
• Periapical abscess – infection at the tip of the tooth root, usually due to untreated decay or pulp infection
• Periodontal abscess – infection in the gums and supporting structures of the teeth
• Gingival infection – localized infection of gum tissue
• Pericoronitis – infection around partially erupted teeth (commonly wisdom teeth)
Signs and symptoms:
• Severe or throbbing tooth pain
• Swelling of the gums, face, or jaw
• Pus discharge or bad taste in the mouth
• Fever and general discomfort
• Difficulty chewing or opening the mouth
• Sensitivity to pressure or temperature
Potential complications:
If untreated, oral infections may spread to surrounding tissues, leading to cellulitis, systemic infection, or, in severe cases, life-threatening conditions. Early intervention is critical to prevent progression.
Management and treatment:
• Immediate dental evaluation
• Drainage of abscess when necessary
• Antibiotic therapy in indicated cases
• Removal of the source of infection (e.g., root canal treatment or extraction)
• Pain management and supportive care
Prevention:
• Maintaining proper oral hygiene
• Regular dental check-ups
• Early treatment of cavities and gum disease
• Avoiding delay in seeking care when symptoms appear

Risk Factors Affecting Oral Health
Oral health is influenced by a combination of behavioral, dietary, and systemic factors. Understanding these risk factors is essential for prevention, early intervention, and long-term maintenance of oral health.
• Poor hygiene habits
Inadequate or inconsistent brushing and flossing allows plaque to accumulate, increasing the risk of dental caries, gingivitis, and periodontitis. Improper technique can further reduce the effectiveness of daily oral care.
• High sugar diet
Frequent consumption of sugary foods and beverages promotes acid production by oral bacteria, leading to enamel demineralization and increased risk of cavities. The frequency of sugar intake is often more harmful than the quantity.
• Smoking
Tobacco use significantly increases the risk of periodontal disease, delays healing, and reduces blood flow to the gums. It also contributes to tooth discoloration, bad breath, and a higher risk of oral cancer.
• Chronic diseases (e.g., diabetes)
Systemic conditions such as diabetes can impair immune response and increase susceptibility to infections, including periodontal disease. Poorly controlled diabetes is strongly associated with more severe and rapidly progressing gum disease.
• Lack of regular dental care
Irregular dental visits prevent early detection and management of oral health issues. Professional cleanings and examinations are essential for removing calculus (tartar) and identifying problems before they become advanced.
Practical Application in Professional Settings
In healthcare-adjacent environments, professionals often perform procedures in close proximity to the face and oral region, where the risk of contamination and infection transmission is elevated. Safe practice requires not only technical skill but also strong awareness of hygiene, screening, and risk management.
Key applications include:
• Maintaining strict hygiene before close-contact procedures
Proper hand hygiene, use of personal protective equipment (PPE), and preparation of a clean workspace are essential to minimize the risk of cross-contamination.
• Recognizing visible signs of oral infection or inflammation
Professionals must be able to identify redness, swelling, lesions, or asymmetry in the oral and perioral area, which may indicate underlying infection or pathology.
• Avoiding procedures when active infection is present
Performing procedures on compromised tissue increases the risk of complications, delayed healing, and spread of infection.
• Educating clients on hygiene-related risks
Clear communication helps clients understand how oral hygiene and health conditions can affect procedure safety and outcomes.
• Reducing cross-contamination risks
This includes proper instrument handling, avoiding contact with contaminated surfaces, and following strict sanitation protocols before and after each client.


When to Avoid or Postpone Procedures
Client safety must always take priority over proceeding with a scheduled service. Procedures should be delayed when risk factors are identified.
Procedures should be postponed if:
• Active oral infection is present
Including abscesses, visible pus, or signs of bacterial infection
• Visible inflammation or lesions are observed
Such as unexplained redness, ulcers, or tissue damage
• Client reports pain or swelling
These symptoms may indicate underlying infection or pathology requiring evaluation
• There are signs of systemic illness
Including fever, fatigue, or recent infection, which may compromise healing and increase risk
Module Summary
Oral health plays a critical role in overall safety, infection prevention, and systemic health. Poor oral hygiene increases bacterial load, contributes to disease, and can impact both individual and public health.
In this module, participants learned:
• The connection between oral health and systemic conditions
• Proper daily hygiene practices and prevention strategies
• Recommended dental care schedules
• Common oral diseases and risk factors
• The importance of recognizing unsafe conditions
• How oral health influences safety in professional environments
Understanding and applying oral health principles strengthens infection prevention, reduces avoidable risks, and supports safer outcomes in healthcare-adjacent practice.
Oral health awareness is an essential component of comprehensive safety and public health strategy.

